Procedures
Angioplasty
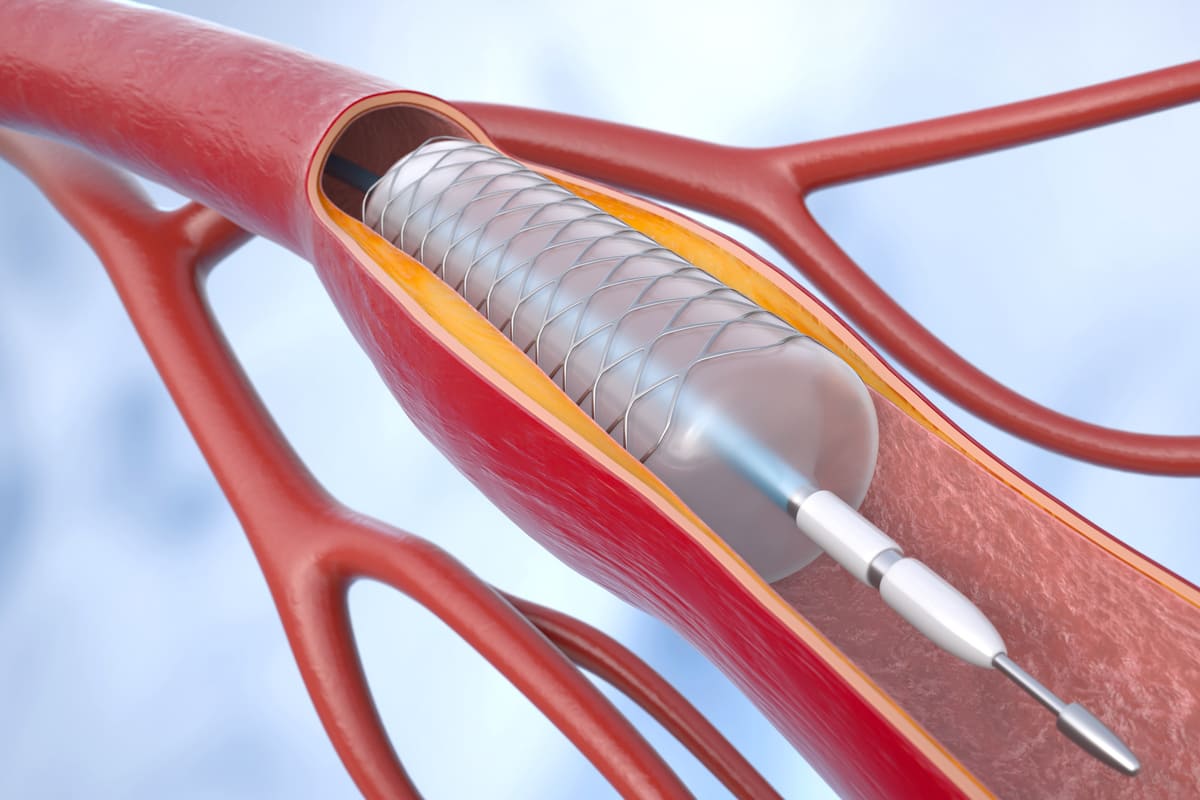
Percutaneous transluminal coronary angioplasty (PTCA), or angioplasty, is an invasive procedure performed to reduce or eliminate blockages in coronary arteries. The goal of PTCA is to restore blood flow to blood-deprived heart tissue, reduce the need for medication, and eliminate or reduce the number of episodes of angina (chest pain).
Opening a blockage, or a plaque, in a coronary artery typically involves the use of an angioplasty balloon. Often, a stent is implanted after angioplasty to keep the artery open and prevent restenosis (re-growth of plaque).
The arteries are accessed through a needle puncture made in the groin (femoral artery) or arm (brachial artery). Usually the femoral artery is used.
More than one blockage can be treated during a single session, depending on the location of the blockages and the patient’s condition. The procedure can take 30 minutes to several hours, depending on the number of blockages being treated.
Indications
Angioplasty is recommended for patients with one or more of the following symptoms:
Blockage (stenosis) of one or more coronary arteries, Angina not well controlled with medications, Angina that disrupts daily activities, occurs at rest (i.e., without exercise or exertion), or recurs after heart attack.
PET
Mid Valley Cardiology is pleased to announce that it now offers the latest diagnostic imaging technology, positron emission tomography, or PET imaging, for heart disease patients. Mid Valley Cardiology offers the only dedicated cardiac PET in the Fresno area. PET imaging is a powerful modality that enables physicians to detect and diagnose coronary artery disease quickly and accurately.
Mid Valley Cardiology has always been a leader in patient care. The addition of PET imaging will make a profound difference in patients’ lives. Not only can we detect heart disease earlier and more accurately, we can learn more quickly whether treatments are working or need to be altered.
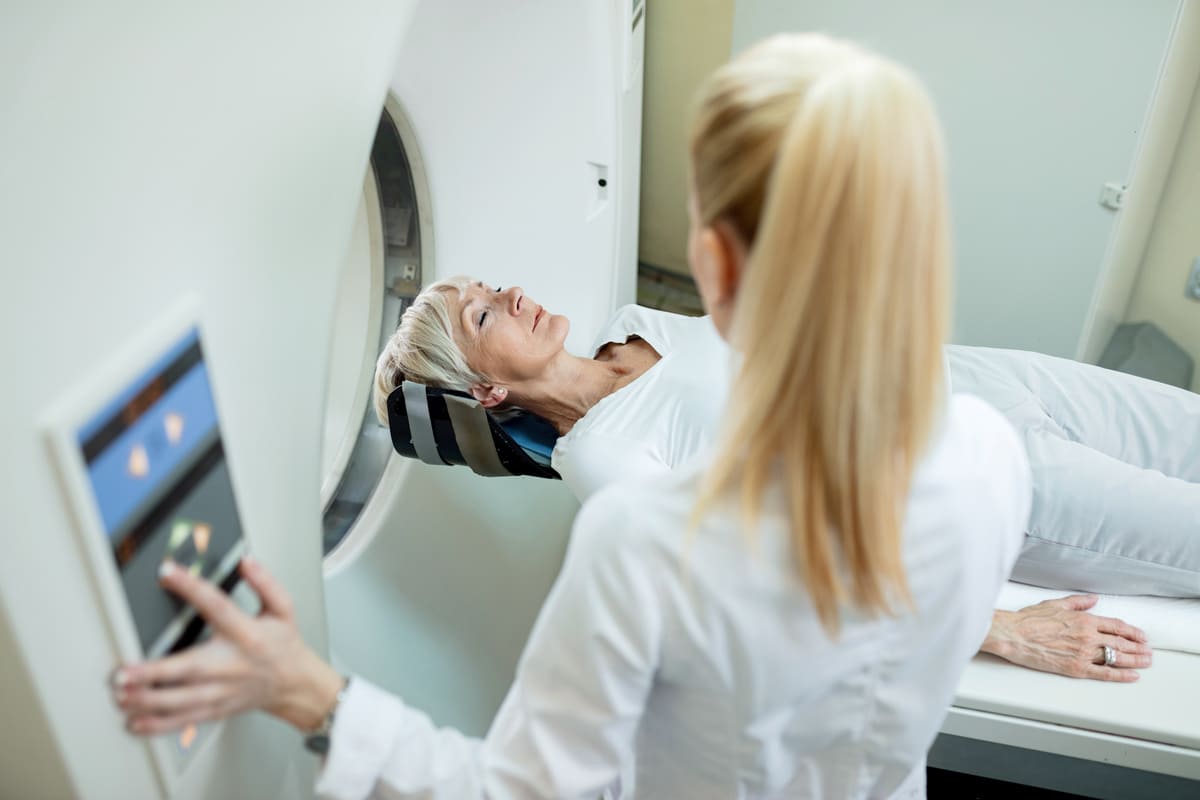
PET studies are convenient and easy for the patient. Scanning begins following the injection of the PET tracer Rubidium 82 which is rapidly taken up by heart muscle cells following the injection. While lying on a comfortable table, the patient moves through the scanner to obtain images of the heart. The entire procedure usually takes 45 minutes. This is compared to the 4-6 hours for single photon emission computed tomography (SPECT).
SPECT has been our only means of performing nuclear myocardial perfusion imaging (MPI) studies until the introduction of our cardiac PET program (September 2010). While SPECT can serve as an effective tool for many patients, PET offers unique advantages that can be especially beneficial for difficult to image patients. PET reduces the potential for attenuation artifacts seen with SPECT imaging, particularly in patients with a significant amount of additional soft tissue (obese, BMI >30, and large breasted women). PET imaging is performed at a fraction of the radiation exposure of SPECT with a much higher accuracy of disease detection (90-95% sensitivity and 95% specificity).
Patients who would especially benefit from PET MPI:
Those who require pharmacologic stress testing
Obese (BMI > 30)
Female (especially patients with large breasts)
Patients likely to have multi-vessel disease
Patients who have had an equivocal SPECT MPI study
EKG
What is it used for?
The ECG is the most commonly performed cardiac test. This is because of the ECG is a useful screening tool for a variety of cardiac abnormalities; ECG machines are readily available in most medical facilities; and the test is simple to perform, risk-free and inexpensive.
How is the ECG performed?
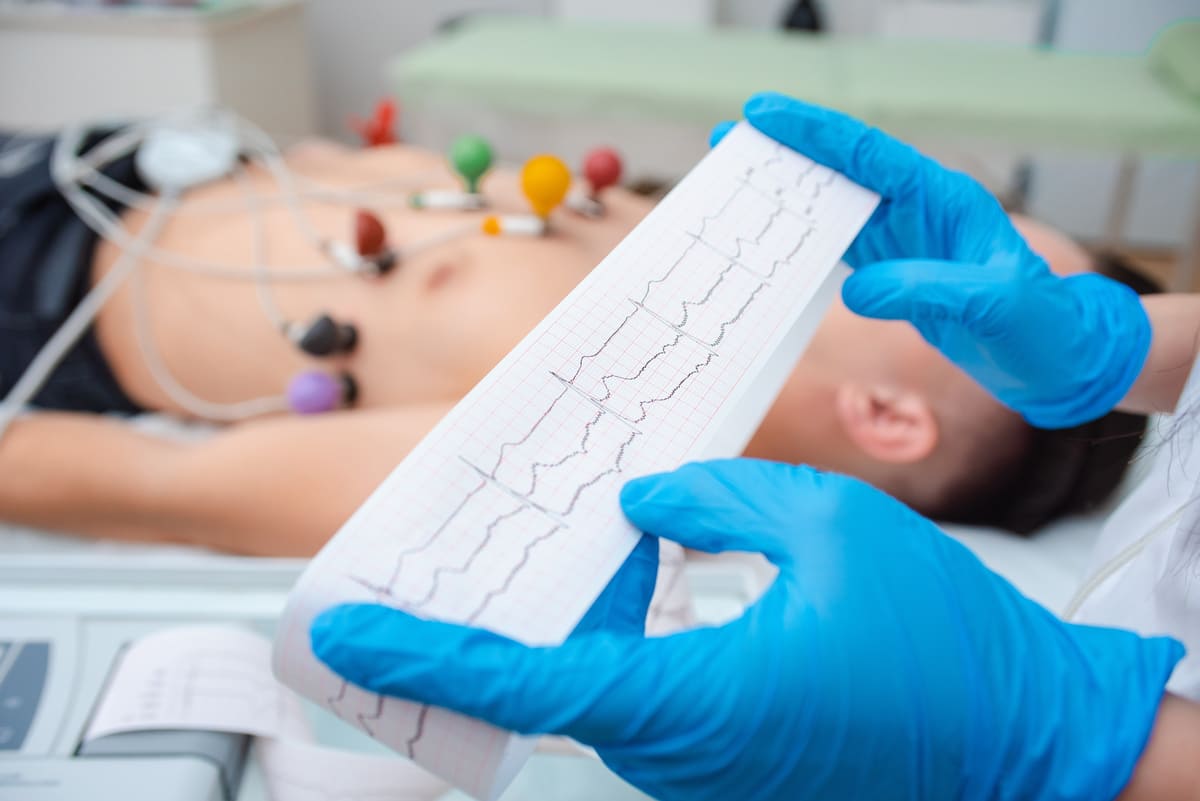
The patient lies on an examination table, and 10 electrodes (or leads) are attached to the patient’s arms, legs, and chest. The electrodes detect the electrical impulses generated by the heart, and transmit them to the ECG machine. The ECG machine produces a graph (the ECG tracing) of those cardiac electrical impulses. The electrodes are then removed. The test takes less than 5 minutes to perform.
What information can be gained from the ECG?
From the ECG tracing, the following information can be determined:
The heart rate, the heart rhythm, whether there are conduction abnormalities, whether there has been a prior heart attack, whether there may be coronary artery disease, whether the heart muscle has become abnormally thickened.
All of these features are potentially important. If the ECG indicates a heart attack or possible coronary artery disease, further testing is often done to completely define the nature of the problem and decide on the optimal therapy. If the heart muscle is thickened, an echocardiogram is often ordered to look for possible valvular heart disease or other structural abnormalities. Conduction abnormalities may be a clue to the diagnosis of syncope (fainting), or may indicate underlying cardiac disease.
Echocardiogram
Echocardiogram is an extremely useful test for studying the heart’s anatomy. It is non-invasive and entirely safe, and when interpreted by well-trained cardiologists, is very accurate.
How is the echocardiogram performed?
The patient lies on a bed or examination table, and the echo technician places a transducer (a device that resembles a computer mouse) over the chest wall. The transducer is moved back and forth across the chest wall, collecting several “views” of the heart. The test takes approximately 30 minutes to complete.
How does the echocardiogram work?
The transducer placed on the chest sends sound waves toward the heart. Like the sonar on a submarine, the sound waves bounce off the cardiac structures (that is, they “echo” of the heart). The sound wave “echos” are collected by the transducer. These returning sound waves are computer-processed, and an image of the beating heart is produced on a television screen. By “aiming” the transducer, most of the important cardiac structures can be imaged by the echocardiogram.
What are some of the variations used with the echocardiogram?
Echocardiograms are sometimes used in conjunction with stress tests. An echo test is made at rest, and then with exercise, looking for changes in the function of the heart muscle when exercise is performed.
Deterioration in muscle function during exercise can indicate coronary artery disease.
A Doppler microphone can be used during echocardiography to measure the velocity of blood flow in the heart. This information can be useful in assessing heart valve function.
What is the echocardiogram good for?
The echocardiogram reveals important information about the anatomy of the heart. It is especially useful for detecting problems with the heart valves. It is also an extremely useful test for evaluating congenital heart disease. The echocardiogram is also a good way to get a general idea of the overall function of the heart muscle.
Pacemaker
What are pacemakers supposed to accomplish?
A pacemaker is a sophisticated electronic device that does two things:
- It analyzes the function of the heart’s own electrical system.
- When necessary, it sends tiny, precisely-timed electrical signals to the heart, to correct certain abnormalities in the heart’s electrical system.
Most pacemakers are designed to correct the bradycardias (the slow ones). Abnormally slow heart rhythms can cause weakness, fatigue, lightheadedness, dizziness, loss of consciousness, or even death. Pacemakers, properly used, effectively eliminate all of these symptoms.
PET studies are convenient and easy for the patient. Scanning begins following the injection of the PET tracer Rubidium 82 which is rapidly taken up by heart muscle cells following the injection. While lying on a comfortable table, the patient moves through the scanner to obtain images of the heart. The entire procedure usually takes 45 minutes. This is compared to the 4-6 hours for single photon emission computed tomography (SPECT).
SPECT has been our only means of performing nuclear myocardial perfusion imaging (MPI) studies until the introduction of our cardiac PET program (September 2010). While SPECT can serve as an effective tool for many patients, PET offers unique advantages that can be especially beneficial for difficult to image patients. PET reduces the potential for attenuation artifacts seen with SPECT imaging, particularly in patients with a significant amount of additional soft tissue (obese, BMI >30, and large breasted women). PET imaging is performed at a fraction of the radiation exposure of SPECT with a much higher accuracy of disease detection (90-95% sensitivity and 95% specificity).
Pacemakers consist of two major parts: the generator and the leads.
Generator
The generator is essentially a tiny, hermetically sealed computer – along with a battery to run it – housed in a titanium container. Most modern pacemaker generators are roughly the size of a 50-cent piece, and approximately three times as thick. The battery life of most pacemaker generators today is 5-8 years.
Lead
The lead is a flexible insulated electrical wire. One end is attached to the generator and the other end is passed through a vein in the heart. Most pacemakers today use 2 leads – one placed in the right atrium and the other in the right ventricle.
How it works
The pacemaker leads detect the heart’s own electrical activity (in the right atrium and right ventricle,) and transmit that information to the pacemaker generator. The generator – which, again, is a computer – analyzes the heart’s electrical signals, and uses that information to decide whether, when, and where to pace. If the heart rate becomes too slow, the generator transmits a tiny electrical signal to the heart, thus stimulating the heart muscle to contract. (This is called pacing.) Pacemakers that have two leads not only keep the heart rate from dropping too low, they can also maintain the optimal coordination between the atria and the ventricles (by pacing the atrium and the ventricle in sequence.)
Thus, pacemakers do not take over the work of the heart – the heart still does its own beating – but instead, pacemakers merely help to regulate the timing of the heart beat.
What devices can interfere with pacemakers?
Home appliances do not interfere with pacemakers, and should not cause any concern whatsoever. (This includes microwave ovens, despite the signs you still see posted in some restaurants.)
Arc welding equipment and other devices that generate powerful magnetic fields can inhibit the function of pacemakers.
MRI scanners can interrupt the pacing function of pacemakers. This problem can often be circumvented by special programming of the pacemaker.
Radiation therapy for cancers can damage the circuits of a pacemaker, and the pacemaker needs to be shielded from the radiation field.
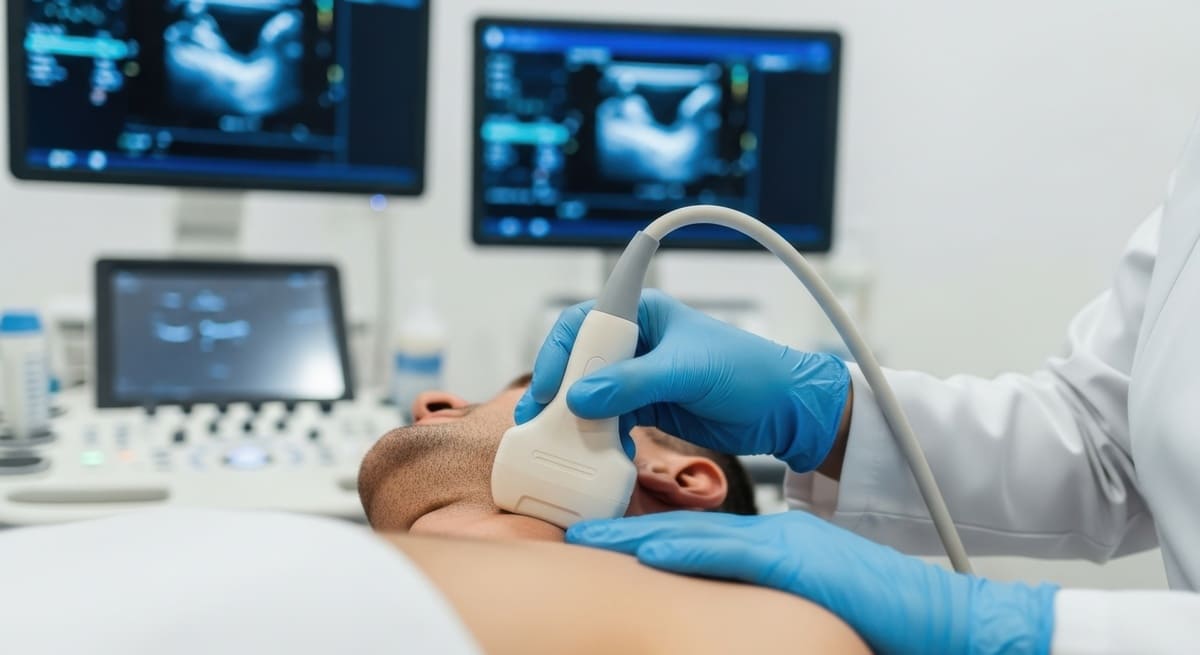
Carotid Ultrasound
Carotid ultrasound is a test that shows the carotid arteries (vessels in the neck that provide blood flow to the brain), as well as how much blood flows and how fast it travels through them. Ultrasound waves – the same ones used in imaging the fetus in a pregnant woman – are used to make an image of the arteries. This image can be used to find out if there is an abnormality or blockage of the carotid arteries that could lead to stroke.
Why do doctors use carotid ultrasound?
Doctors often use carotid ultrasound on patients who have had a stroke or who might be at high risk for a stroke. Narrowing of the carotid arteries – often caused by cholesterol deposits – and blood clots can be detected using this procedure. These conditions can cause problems with the blood flow to the brain and lead to a stroke. The actual blood flow through the carotid arteries can also be imaged by this test.
What happens during carotid ultrasound?
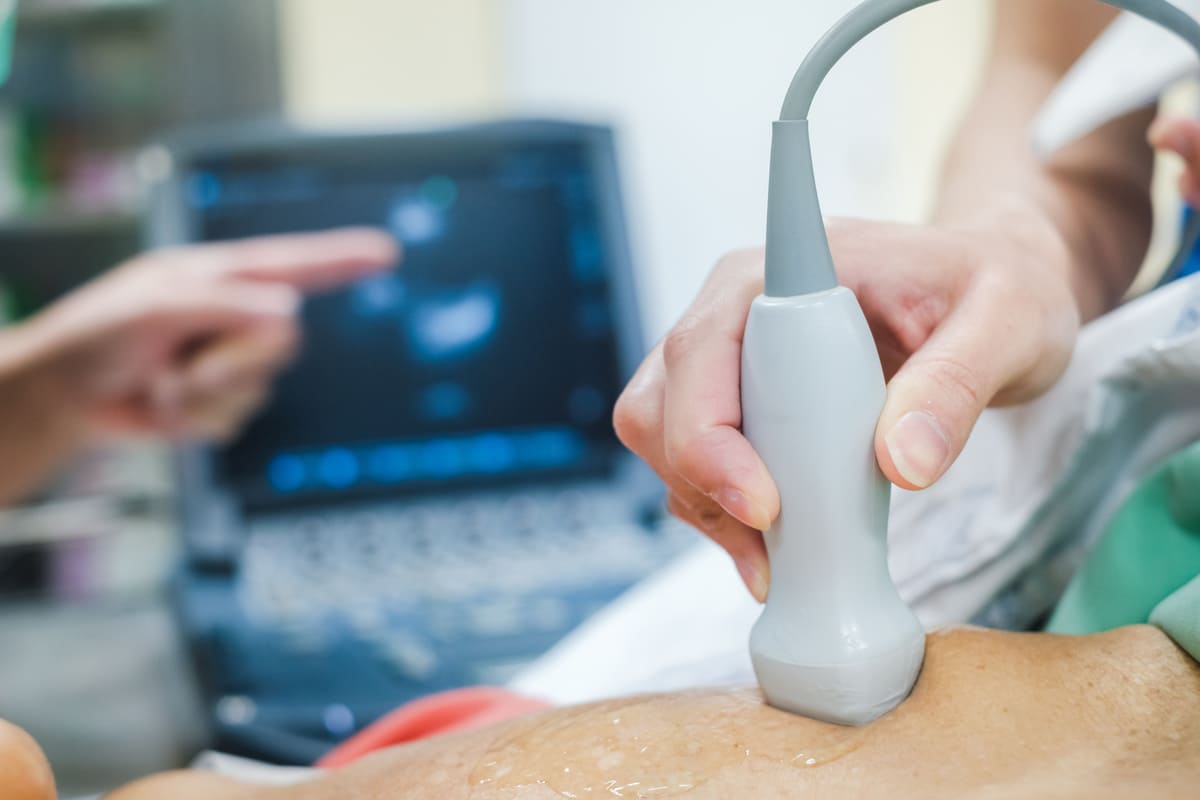
You will be asked to lie down on an examination table. The technician will place a clear gel on the area of the neck where the carotid artery is located. The gel is simply a lubricant that allows the transducer (a device that both puts out and detects ultrasound signals) to slide around easily on your skin. When the transducer is placed against the skin, an image of the artery is shown on a video screen. To view the arteries from many different angles, your doctor will re-position the transducer several times. Because blood is flowing through the artery, a sound similar to your heartbeat will be heard. The procedure is repeated for the carotid artery on the other side of the neck. A carotid ultrasound usually only takes 15 to 30 minutes to complete.
What are the risks of carotid ultrasound?
Since the procedure is done without entering the body and does not use dyes or x-rays, there is no risk or pain involved in having a carotid ultrasound.
How does carotid ultrasound work?
The transducer emits high frequency, ultrasound waves that pass into the body and bounce off the carotid arteries and the red blood cells moving through them. The transducer detects the different reflections of the sound waves, which are then measured and converted by a computer into live pictures of the arteries and the blood flow.
Cardioversion
What is an electrical cardioversion?
Cardioversion is a brief procedure where an electrical shock is delivered to the heart to convert an abnormal heart rhythm back to a normal rhythm. Most elective or “non-emergency” cardioversions are performed to treat atrial fibrillation or atrial flutter, benign heart rhythm disturbances originating in the upper chambers (atria) of the heart. Cardioversion is used in emergency situations to correct a rapid abnormal rhythm associated with faintness, low blood pressure, chest pain, difficulty breathing or loss of consciousness.
Why do I need a cardioversion?
Each normal heartbeat starts in an area of the heart known as the sinus node which is located in the upper right chamber of the heart (right atria). The sinus node contains specialized cells that send an organized electrical signal through the heart resulting in a perfectly timed, rhythmic heartbeat. In patients with atrial fibrillation, however, the atria fibrillate (or “quiver”) due to chaotic electrical signals that circulate throughout both aria. This typically results in a fast and irregular heartbeat. While some patients have no symptoms, others may experience shortness of breath, lightheadedness and fatigue.
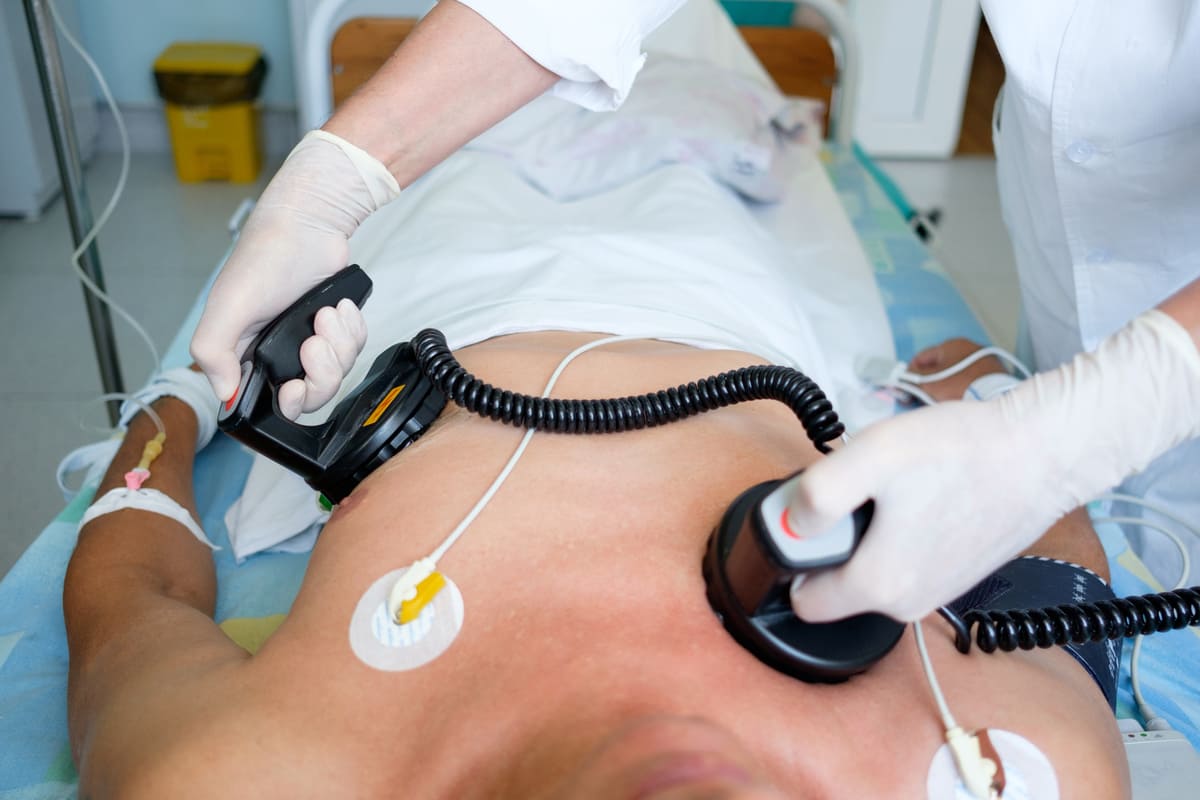
Electrical cardioversion is a procedure whereby a synchronized (perfectly timed) electrical shock is delivered through the chest wall to the heart through special electrodes or paddles that are applied to the skin of the chest and back. The goal of the cardioversion is to disrupt the abnormal electrical circuit(s) in the heart and to restore a normal heartbeat. The shock causes all the heart cells to contract simultaneously, thereby interrupting, thereby interrupting and terminating the abnormal electrical rhythm (typically fibrillation of the atria) without damaging the heart. This split second interruption of the abnormal beat allows the heart’s electrical system to regain control and restore a normal heartbeat.
An electrical cardioversion is performed in a hospital setting. A cardiologist, a nurse and/or an anesthesiologist are present to monitor your breathing, blood pressure and heart rhythm. Special cardioversion pads are placed on your chest and back (or alternatively, both pads can be placed on the front of the chest). The pads are connected to an external defibrillator by a cable. The defibrillator allows the medical team to continuously monitor your heart rhythm and to deliver the electrical shock to restore your heart’s rhythm back to normal.
Holter Monitor
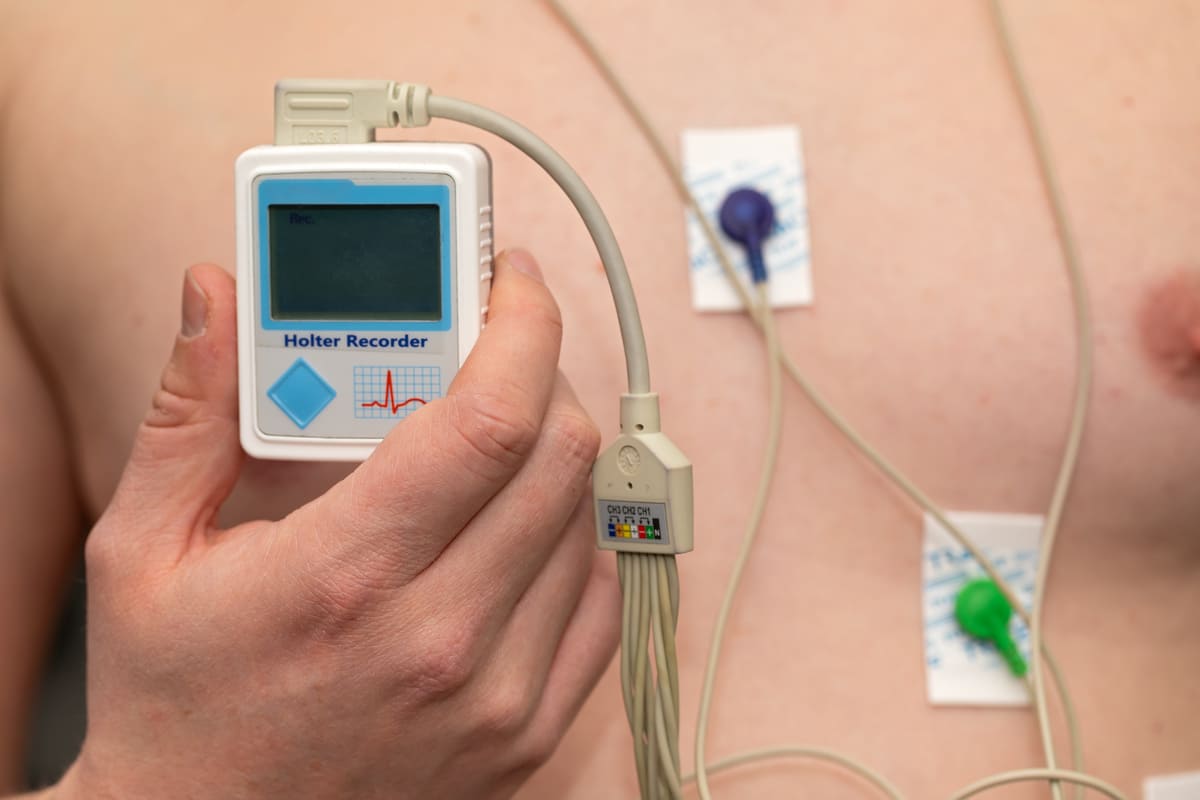
What is a Holter Monitor?
Holter monitoring is a continual monitoring of heart rate and rhythm during your usual daily activities over a predetermined length of time, usually a 24-hour period.
Why this test may be performed?
A Holter monitor is used to identify heart rhythm disturbances, which may come and go at various times throughout the day or night. It is often used to correlate any abnormal heart rhythm with a person’s symptoms, like dizziness, palpitations, shortness of breath or chest pain.
What this test involves?
Electrodes are placed on the front of the chest and the electrode wires are then attached to a small portable, battery-operated recorder. The recorder is held in place by a belt that can be worn around the wait. The recorder continuously records and stores the heart rhythm for 24 hours. The person is encouraged to continue their usual daily activities. During this time period, the person wearing the device maintains a written log. Symptoms (for example, palpitations, dizziness, and shortness of breath) are written in the log, noting the exact activity and time they occur. Once the monitor has been removed, a physician analyzes the heart rhythm and activity log.
What are the risks/precautions for this test?
A Holter monitor is a non-invasive test. It is painless and not associated with any risks to the patient. It is advisable to shower or bathe before the electrodes are applied to the chest, since you will not be able to do either of these activities while the test is in progress.
What the results may tell you?
A Holter monitor may detect a disturbance in heart rhythm that is not evident on a single, resting electrocardiogram tracing. It allows the physician to correlate specific patient symptoms with the electrical activity of the heart. A Holter monitor can detect rhythm disturbances that are transient or intermittent in nature.
Event Monitor
What is a cardiac event monitor?
A cardiac event monitor is a small recorder that records your heart activity only when you want it to. When you experience symptoms you activate the monitor to make a brief recording of your heart’s electrical activity. Patients wear Event Monitors for 30 days.
Why do I need a cardiac event monitor?
Event monitors help your doctor to diagnose problems that don’t happen often enough for an EKG or Holter monitor to record. They are very useful to your doctor in diagnosing problems with your heart rhythm (arrhythmias) that happen infrequently.
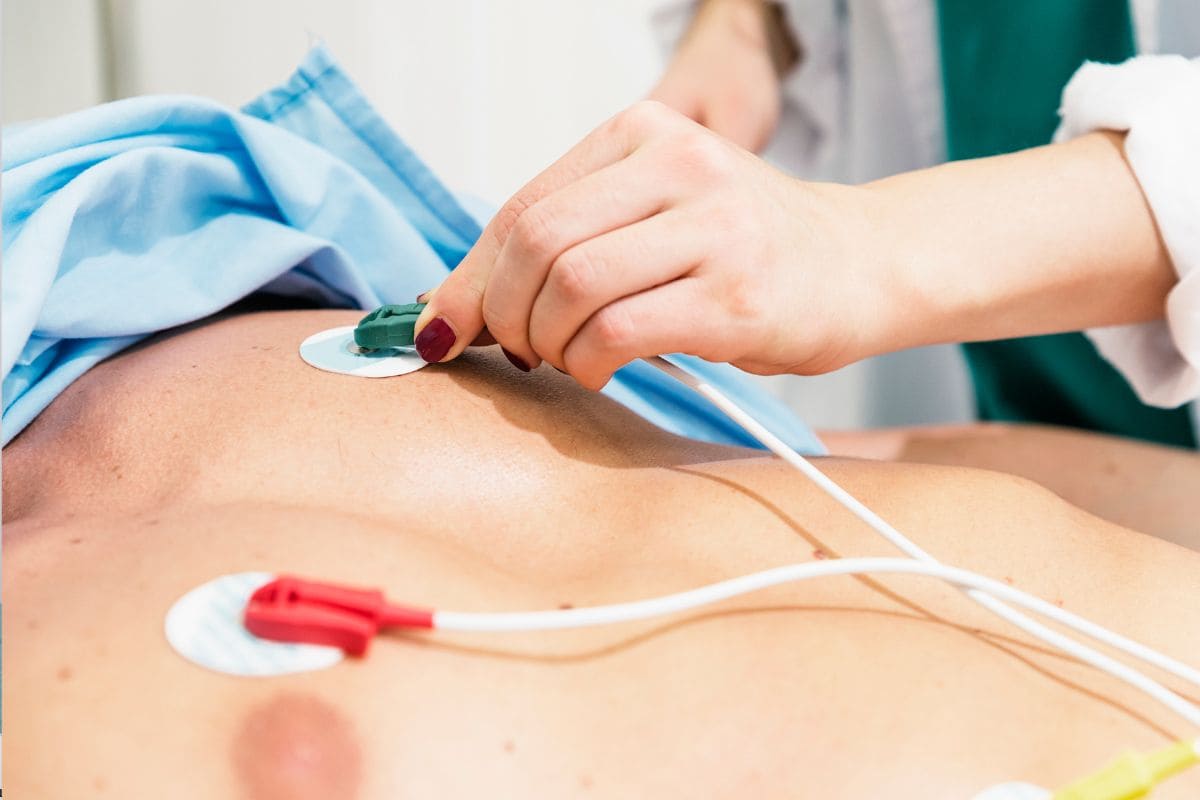
Using The Cardiac Event Monitor
The electrodes are attached to your chest and connected by wires to the recorder. Worn day and night, the recorder continuously scans your heart’s electrical activity. When you experience symptoms, you activate the recorder by pressing a button. The device records and stores several minutes of EKG data before, during and after an event. Then you transmit the stored data over a telephone to a receiving center, who transfers the information to your doctor.
Segmental Pressures
What are segmental pressures?
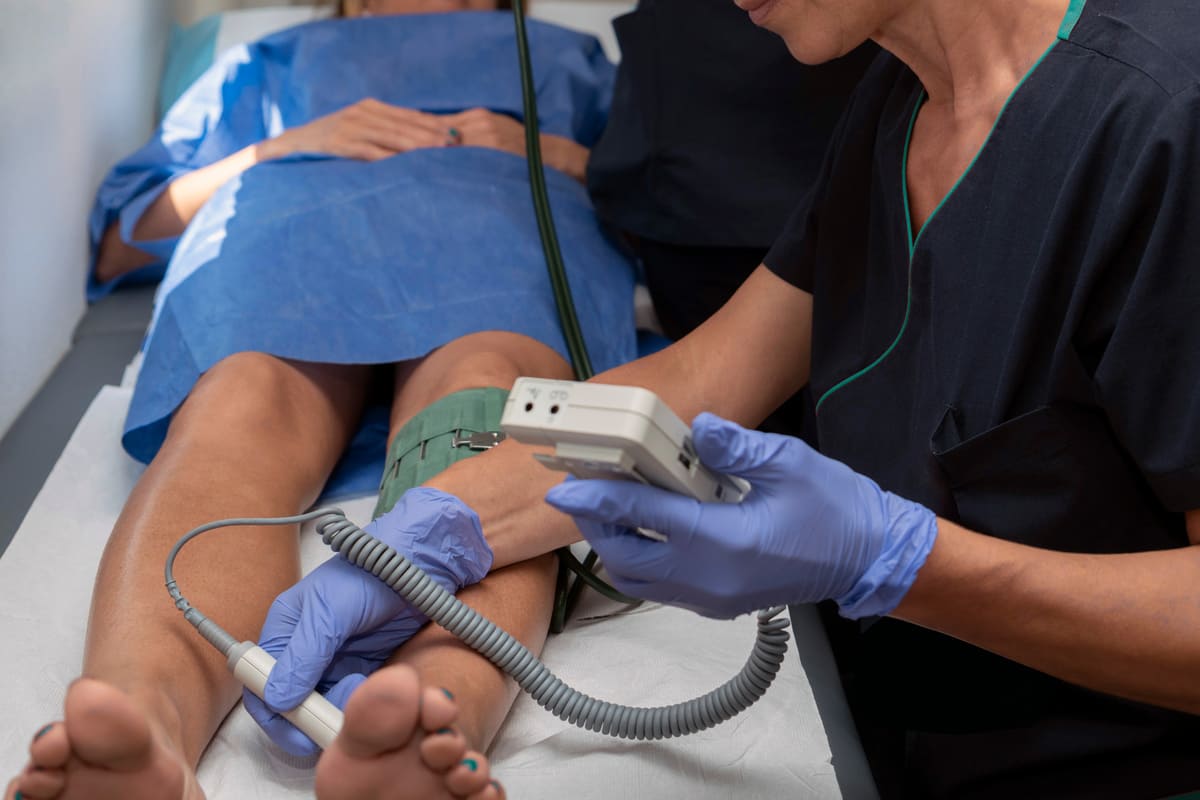
Segmental pressures are a non-invasive measurement of bilateral leg pressures with blood pressure cuffs and a Doppler/PPG prove ultrasound detector. The cuffs and Doppler/PPG probe ultrasound identify and quantify significant obstructive arterial lesions in the legs. In other words, the test assists in identifying the possible location of narrowing and/or blockage of the arterial blood supply in the legs.
What happens during the test?
You will be placed on an exam table and bilateral arm pressures will be taken. Then 4 cuffs will be placed on each leg at the ankle, below the knee, above the knee and high thigh. The cuff will inflate until the pulse signal disappears at which time the cuff will then slowly release the pressure until the pulse returns. Blood pressures are obtained by using a special microphone or Doppler transducer to listen to the pulses at your ankles. The process will continue up the leg until all cuffs have been inflated. The high thigh pressure may cause some discomfort with inflation.
How do I prepare for the test?
There are no special instructions for this test. You will be asked to remove clothing and given a drape. If you are more comfortable you may bring exercise shorts to wear during the procedure.